요약배경/목적:담관암의 완치를 위해서는 수술적 절제가 필요하다. 하지만 불행히도 담관암은 초기에 임상 증상이 거의 없으므로 수술이 가능한 초기에 발견되는 경우는 매우 드물다. 그러므로 대부분의 담관암 환자에게서는 완치를 위한 수술적 절제보다 증상완화와 생명연장을 위한 고식적인 치료를 시행하게 된다. 이번 연구는 간문부담관암의 고식적인 치료에서 관내근접치료의 치료 효능을 알기 위하여 시행하였다.
방법:연구에 참여한 모든 관문부담관암 환자에게 방사선 치료를 시행하기 전에 폐쇄성 황달을 치료하기 위하여 담관 스텐트를 삽입하였다. 총 12 명의 간문부담관암 환자는(group 1) 외부방사선치료만을 이용하여 고식적인 치료를 시행하였고 9명의 환자에게서는(group 2) 외부방사선치료와 관내근접치료를 함께 시행하였다. 두 군의 생존기간과 스텐트 개통기간을 통계학적으로 비교하였다.
결과:환자들의 생존기간은 통계적으로 큰 차이를 보이지 않았다. 평균 생존기간은 group 1에서 353일, group 2에서는 224일이었다(p=0.172). 스텐트 개통기간도 두 군 간의 특별한 차이를 보이지 않았다(p=0.62). 또한 환자의 나이, 스텐트 삽입 방법 등의 비교에서도 환자의 생존기간과 스텐트의 개통기간에 영향을 미치는 인자를 찾을 수 없었다. 그러나 방사선 치료에 사용된 총 방사선 양이 증가 할수록 환자의 생존기간이 증가하는 경향을 확인할 수 있었다(Spearman correlation coefficient=0.65, p=0.065).
AbstractBackground/Aims:The aim of this study is to assess the therapeutic benefits of a combination of external beam radiation therapy (EBRT) and intraluminal brachytherapy (ILBT) in hilar cholangiocarcinoma as palliative therapy.
Methods:A total of 21 patients with hilar cholangiocarcinoma were included. Only 12 patients were treated with EBRT (group 1), and only nine patients were treated with EBRT and ILBT (group 2). The survival data and stent patency period were measured in both groups and the results were compared.
Results:No statistically significant difference in patient survival was observed between the two groups. The median survival period of group 1 was 353 days and that of group 2 was 224 days. Also, stent patency did not differ significantly between groups. The period for group 1 was 250 days, and that of group 2 was 133 days. In addition, there were no other factors influencing patient survival and stent patency period. However, patient survival tended to increase with increase in the amount of irradiation dose (Spearman’s correlation coefficient=0.65, p=0.065).
INTRODUCTIONCholangiocarcinoma is the primary malignant tumor of the bile ducts which originates from cholangiocytes [1]. Surgical resection is the only curative therapy. Unfortunately, due to lack of symptoms until late in the disease, the majority of patients present with unresectable disease, typically resulting in advanced cholangiocarcinoma at the time of diagnosis. In addition, advanced age, poor performance status, acute illness, and/or systemic disease are considered inoperable in many cases [2,3]. In particular, in hilar cholangiocarcinoma, primary invasion of the portal vein and metastasis to the hepatic lobes occurs so frequently that surgical resection is impossible, and it is associated with a poor prognosis [4]. Biliary stent insertion using percutaneous transhepatic biliary drainage (PTBD) or endoscopic retrograde biliary drainage is a widely accepted palliative procedure with the intent of symptomatic relief, such as obstructive jaundice [5,6]. Biliary stent insertion could result in slightly improved prognosis of patients by prevention of biliary stasis and hepatic failure. However, dysfunction of a biliary stent often occurs due to clogging of the stent lumen by biliary sludge, tumor ingrowth, or tumor overgrowth [7]. In order to reduce the incidence of dysfunction of a biliary stent, radiation therapy (RT) is used. In addition, RT is also used for the purpose of improving the prognosis of patients with cholangiocarcinoma because cholangiocarcinoma does not show a good response to chemotherapy, and effective regimens have not been studied well [8].
The types of RT used include External beam radiation therapy (EBRT) and intraluminal brachytherapy (ILBT); these RT methods have been used separately or in conjunction. EBRT can reduce the tumor volume; however, there is a considerable problem in that approaching the tumoricidal dose is difficult because of the radiation tolerance limits of the adjacent organs[9]. ILBT has been increasingly applied in order to minimize radiation exposure to the adjacent organs and to apply localized high dose radiation on the tumor [10]. Many studies have demonstrated and accepted that treatment of advanced inoperable cholangiocarcinoma using only ILBT has limited effectiveness due to frequent recurrences within the non-irradiated portion of the bile duct. Therefore, treatment with ILBT only has been used restrictively in small carcinomas that do not spread beyond the extrahepatic bile duct [11]. However, the effect of combination of EBRT with ILBT remains controversial. Shin et al. [9] reported that combined use of EBRT and ILBT is an effective method for improving the treatment outcome in patients with inoperable carcinoma of the extrahepatic bile ducts. On the other hand, according to a recent retrospective trial, RT improved patient prognosis and the patency of uncovered metallic stents, however, ILBT provided no additional benefits [12].
Consequently, the aim of this study is to prove the validity of ILBT with comparison of the effect of EBRT along with ILBT and the effect of EBRT alone in patients with advanced hilar cholangiocarcinoma. In addition, we attempted to determine how the stent patency was improved by ILBT.
METHODS1. PatientsBetween September 2004 and February 2008, 63 patients with pathologically confirmed hilar cholangiocarcinoma that did not metastasize to other organs were treated at Inha University Hospital and retrospectively enrolled in this study. Bile duct cancer was diagnosed by pathological examination, clinical course, or imaging results. The tumor location was established using ultrasonography, computed tomography (CT), endoscopic retrograde cholangiopancreatography (ERCP), and/or percutaneous transhepatic cholangiography. All patients had an obstructive jaundice and required drainage. In order to resolve the obstructive jaundice, we first performed endoscopic drainage, such as a plastic stent or placement of a nasobiliary drainage tube. If endoscopic drainage was not possible, we performed bile drainage using percutaneous transhepatic biliary drainage under fluoroscopic guidance. Of these 63 patients, 32 patients were excluded. Six patients refused treatment; 23 patients were treated with curative surgery. Three patients underwent the Cyberknife. Two patients could have undergone curative resection, however, they refused to undergo surgery because of their old age and they were treated with EBRT instead, according to their wish. We enrolled these patients in our study. All enrolled patients (n=31) were divided into two groups according to the RT technique. Fifteen patients decide to undergo treatment with EBRT, however, three patients who stopped by their own decision at the beginning of treatment were excluded. Although 16 patients were supposed to undergo treatment with ILBT along with EBRT, seven patients were excluded because they did not undergo EBRT after ILBT. Eventually, 21 patients with hilar cholangiocarcinoma were enrolled in this study. After jaundice had improved, all registered patients underwent exchange of biliary drainage with metal stents, which were placed through the obstructive lesion for maintenance of biliary tracts. Placement of a metal stent through the same route with biliary drainage was attempted. In one patient, placement of the stent using the same route used with the endoscopic method failed, therefore, the patient underwent stent placement using PTBD. Twelve patients were treated with EBRT alone (Group 1) and nine patients were treated with combined EBRT and ILBT (Group 2) (Fig. 1). A summary of the patients’ characteristics is shown in Table 1.
2. Radiation therapyEBRT was performed using a 10-MV X-ray unit, using the typical four-field box technique. Patients received a total dose of 32.4 to 59.4 Gy (median, 47.4 Gy), five fractions weekly, with 1.8 Gy per fraction, which was delivered to the isocenter of the treatment volume. The volume of EBRT included both the primary tumor bed and the regional lymph nodes.
ILBT was performed using 192Ir, which was positioned in order to encompass the tumor with an approximate 2-cm margin proximally and distally. The median dose delivered was 18 Gy with 6 Gy per fraction and was performed three times.
3. Follow upPatient symptoms and blood tests were assessed each time the patient was admitted, and CT was taken every three months. When hepatic-biliary enzymes were increased or patients developed additional symptoms, we performed an additional CT for estimation of stent patency. We followed the clinical courses of patients, and we estimated the results of RT until May 2013.
4. End pointThe first end point was patient death until May 2013. Patient survival period was measured from the date of diagnosis to the date of death. If the patient could not be followed, we adjusted the survival period from the date of diagnosis to the final hospital visiting date. Once the patient was alive until end of the investigation, we estimated the survival period from the date of diagnosis until the investigation was completed. The second end point was stent patency. Stent occlusion was defined by cholangiography. If cholangiography could not be performed, stent occlusion was defined by CT with symptoms of patients. The stent patency was measured from the date of placement until the date of occlusion. If the patient died with a remaining patent stent, the data on stent patency were censored.
5. Statistical evaluationComparisons between groups were evaluated using Kaplan-Meier, and statistical significance was evaluated using a log-rank test. The Mann-Whitney U-test was used for comparison of quantitative variables. The Spearman rank-order correlation coefficient was also used for comparison of irradiation dose with tendency of survival period and stent patency. Multivariate analysis using Cox regression analysis was also performed for evaluation of the prognostic significance of the covariates. p-values<0.05 were considered significant for all statistical analysis.
RESULTS1. Characteristics of the patientsBetween two groups, there were no differences in the basic characteristics of the patients and method of biliary stent placement. The median age of patients in group 1 was 70.5 years and that of patients in group 2 was 72 years. Male to Female ratio was 1:1 (group I) and 2:1 (group II). Cancer staging was estimated using Bismuth classification. When the patients were classified according to Bisthmus classification, five patients had Bisthmus type I, one patient had type II, 11 patients had type IIIa and IIIb, and four patients had type IV. Insertion of the stent was performed in two ways, endoscopic route and percutaneous route. Stent placement was performed through the oral route in 10 patients, percutaneous route in 10 patients, and both methods were used in one patient. The number of stents placed in the patient in order to resolve the obstructive jaundice was decided by the operator. The number of stents used was 1 to 3. Eleven patients needed only one stent, eight patients needed two stents, and two patients needed three stents until the malignant jaundice was resolved. The total irradiation dose was the only factor of significant difference between the two groups. Patients in group 2 received a larger irradiation dose than those in group 1 (p=0.001).
2. Patient survivalOverall median survival period was 345 days (range: 106- 938 days). The median survival period of group 1 was 353 days (range 153-898 days) and that of group 2 was 224 days (range 106-938). No statistically significant difference was observed between group 1 and group 2 (p=0.172, Fig. 2). Cox regression analysis was performed for evaluation of factors, including age, sex, number of stents placed, stage, and stent insertion route, which could affect the survival period of patients. However, no correlation showed between these factors and survival period.
4. Complications of radiotherapyGastric ulcer was observed in three patients, two in group 1, and one in group 2. All the patients with gastric ulcer were treated with anti-ulcer medication, and were treated completely. They did not require hospital admission and were treated in the outpatient clinic. Except gastric ulcer, there was no other complication induced by RT.
DISCUSSIONDespite the low incidence of hilar cholangiocarcinoma, it is a dreadful tumor because the diagnosis is commonly not made until the disease has advanced. Surgical treatment of the advanced hilar cholangiocarcinoma which is only curative treatment, such as hepatectomy and liver transplantation, is usually impossible [1,2,13]. Unfortunately, the median survival period of patients with advanced hilar cholangiocarcinoma is less than one year [14]. Therefore, variable methods of palliative treatment for improved prognosis are still being developed and used in the clinical field. In particular, RT and biliary stent are the most important types of palliative therapy in advanced hilar cholangiocarcinoma. Biliary stent could solve the cholestasis caused by bile duct obstruction, and RT is known to have the ability to improve the prognosis of cholangiocarcinoma by local control of cancer and maintenance of biliary stent patency, although bile duct cancer has a low sensitivity to RT [11]. ILBT is also used on the assumption that it might have an effect on improving the prognosis by a mechanism similar to that of RT [15]. However, based on the results of past studies, the effect of ILBT in cholangiocarcinoma has been controversial. Zimmon et al. [16] initially introduced ILBT as part of a treatment regimen for patients with inoperable tumors; the iridium wire source, which was placed through PTBD in four patients, provides symptomatic palliation and significant tumor control. Shin et al. [9], who also reported similar research results supporting the effect of ILBT, reviewed 31 patients with extrahepatic bile duct cancer treated with either EBRT (n=17) or EBRT plus ILBT (n=14). The median survival period was nine months for patients treated with EBRT plus ILBT, and five months for those who received EBRT alone. On the other hand, Isayama et al. [12] reported the opposite results. Seventeen patients underwent EBRT alone and 11 patients underwent EBRT plus ILBT. Comparison of survival time and stent patency in the EBRT alone and EBRT plus ILBT groups showed no significant difference in survival time or for stent patency between groups. The effect of ILBT in hilar cholangiocarcinoma has been debated in this way. We thought that our result would be helpful in making a conclusion. Results of our study also showed that ILBT combined with EBRT did not offer a survival advantage and a longer stent patency period. We believed that the result occurred by irradiation dosage of EBRT. According to the study reported by Alden and Mohiuddin [17], high-dose radiation of more than 55 Gy showed significantly better survival compared with those who received smaller doses in unresectable cases. In a study of patients treated for cholangiocarcinoma with EBRT and ILBT, they reported that 48% of patients who received high-dose radiation experienced an extended two-year survival. Based on this result, we attempted to verify the statistical significance between the survival rate and radiation amount. According to spearman rank-order correlation between irradiation dose and survival period, tendency of survival expectancy increased as irradiation dose was increased, although the result does not have statistical significance (Spearman’s correlation coefficient=0.65 p=0.065). We also attempted to determine the cut-off point of the effective radiation dose; however, it was impossible because the number of patients was too small to estimate. As a result, administration of the maximum irradiation dose might be an important factor in improving the patient survival period in treatment of inoperable cholangiocarcinoma, regardless of the method of radiation. However, this outcome was based on preliminary data using data from a small number of enrolled patients. Therefore, further studies will be needed in order to confirm our result or hypothesis. In conclusion, the current study has shown that a combination of EBRT and ILBT does not have a benefit for prolongation of patient survival and maintenance of stent patency when compared to EBRT alone. We assumed that the irradiation dose would be the most important factor in control of hilar cholangiocarcinoma in palliation therapy regardless of the method of RT.
REFERENCES2. Gibby DG, Hanks JB, Wanebo HJ, et al. Bile duct carcinoma. Diagnosis and treatment. Ann Surg 1985;202:139-144.
4. Zhimin G, Noor H, Jian-Bo Z, Lin W, Jha RK. Advances in diagnosis and treatment of hilar cholangiocarcinoma - a review. Med Sci Monit 2013;19:648-656.
5. Lee CK, Barrios BR, Bjarnason H. Biliary tree malignancies: the University of Minnesota experience. J Surg Oncol 1997;65:298-305.
7. Jaganmohan S, Lee JH. Self-expandable metal stents in malignant biliary obstruction. Expert Rev Gastroenterol Hepatol 2012;6:105-114.
8. Ramírez-Merino N, Aix SP, Cortés-Funes H. Chemotherapy for cholangiocarcinoma: An update. World J Gastrointest Oncol 2013;5:171-176.
9. Shin HS, Seong J, Kim WC, et al. Combination of external beam irradiation and high-dose-rate intraluminal brachytherapy for inoperable carcinoma of the extrahepatic bile ducts. Int J Radiat Oncol Biol Phys 2003;57:105-112.
10. Kamada T, Saitou H, Takamura A, Nojima T, Okushiba SI. The role of radiotherapy in the management of extrahepatic bile duct cancer: an analysis of 145 consecutive patients treated with intraluminal and/or external beam radiotherapy. Int J Radiat Oncol Biol Phys 1996;34:767-774.
11. Kurosaki H, Karasawa K, Kaizu T, et al. Intraoperative radiotherapy for resectable extrahepatic bile duct cancer. Int J Radiat Oncol Biol Phys 1999;45:635-638.
12. Isayama H, Tsujino T, Nakai Y, et al. Clinical benefit of radiation therapy and metallic stenting for unresectable hilar cholangiocarcinoma. World J Gastroenterol 2012;18:2364-2370.
13. Hassoun Z, Gores GJ, Rosen CB. Preliminary experience with liver transplantation in selected patients with unresectable hilar cholangiocarcinoma. Surg Oncol Clin N Am 2002;11:909-921.
14. Jarnagin WR, Fong Y, DeMatteo RP, et al. Staging, resectability, and outcome in 225 patients with hilar cholangiocarcinoma. Ann Surg 2001;234:507-517.
15. Chan SY, Poon RT, Ng KK, Liu CL, Chan RT, Fan ST. Long-term survival after intraluminal brachytherapy for inoperable hilar cholangiocarcinoma: a case report. World J Gastroenterol 2005;11:3161-3164.
16. Zimmon DS, Bursa J, Chang J, Clemett AR. The management of hepatic duct cancer with percutaneous transhepatic biliary stent and intraluminal irradiation. Gastroenterlogy 1979;77:49.
Fig. 1.Distribution of patients with advanced cholangiocarcinoma. EBRT, external beam radiation therapy; ILBT, intraluminal brachytherapy. 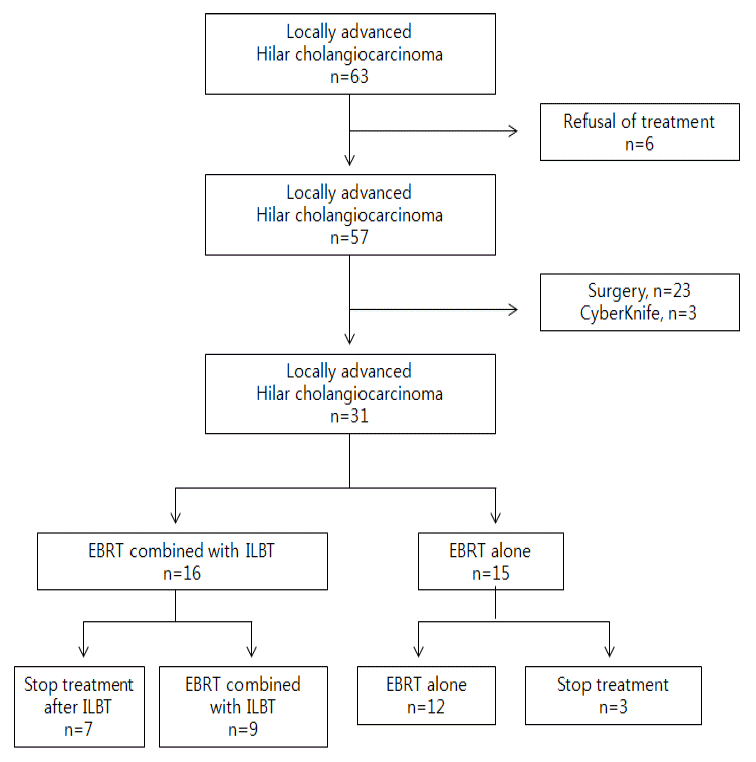
Fig. 2.Cumulative survival rates of Group 1 and Group 2. Cumulative survival periods were calculated using the Kaplan Meier method and compared using the log rank test. No signicant difference was observed between the two groups. EBRT, external beam radiation therapy; ILBT, intraluminal brachytherapy. 
Fig. 3.Cumulative stent patency rates of Group 1 and Group 2. Cumulative stent patency rates were calculated using the Kaplan Meier method and compared using the log rank test. No signicant difference was observed between the two groups. EBRT, external beam radiation therapy; ILBT, intraluminal brachytherapy. 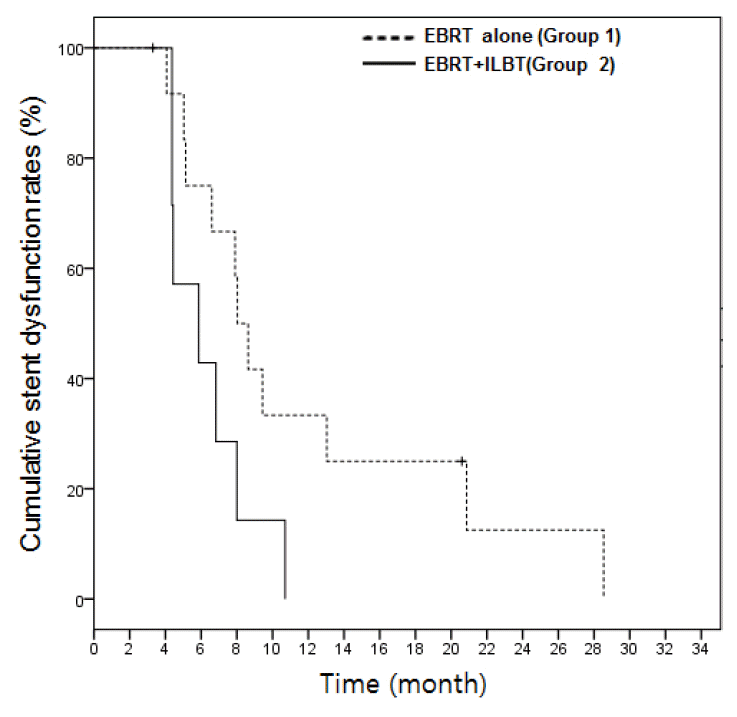
Table 1.Patient characteristics
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||