INTRODUCTION
Mirizzi’s syndrome (MS) is an important and rare complication of gallstone disease, in which an impacted gallstone in the cystic duct or gallbladder (GB) neck compresses the common bile duct (CBD) or the common hepatic duct (CHD), resulting in impediment and jaundice. The incidence of MS among patients that have undergone cholecystectomy is approximately 0.7-1.4% [1]. MS is often difficult to diagnose before surgery, and is normally treated surgically by open cholecystectomy or laparoscopic cholecystectomy with T-tube placement with choledochotomy [2]. However, patients with history of biliary surgery are more difficult to treat with surgically, because of the risks of scarring and adhesion introduced by previous surgery [3]. Accordingly, other less invasive techniques have been tried.
Improvements in endoscopic techniques have prompted the use of endoscopy for the treatment of MS. This report describes the successful treatment of a difficult, cystic duct stone in a patient with post-cholecystectomy MS by endoscopic mechanical lithotripsy (ML).
CASE REPORT
A 37-year-old man presented with epigastric pain of duration one day. He had undergone laparoscopic cholecystectomy 3 months previously due to acute cholecystitis. Initial vital signs were; blood pressure 170/80 mmHg, heart rate 75 beats/min, respiratory rate 18 breaths/min, and body temperature 36.5℃. Physical examination revealed icteric sclera and tenderness in the epigastric area and right upper quadrant. Laboratory findings were as follows; alkaline phosphatase 453 IU/L (103-335), AST 187 IU/L (7-38), ALT 580 IU/ L (4-43), total bilirubin 5.9 mg/dL (0.1-1.3), direct bilirubin 2.9 mg/dL (0.1-0.4), serum albumin 4.4 g/dL (3.1-5.2), white blood cell 5.8×103/μl (4-10), hemoglobin 15.1 g/dl (13.1-17.5), polymorphonuclear neutrophils 67.8% (40-74), amylase 56 IU/L (7-60), and lipase 30 IU/L (7-60).
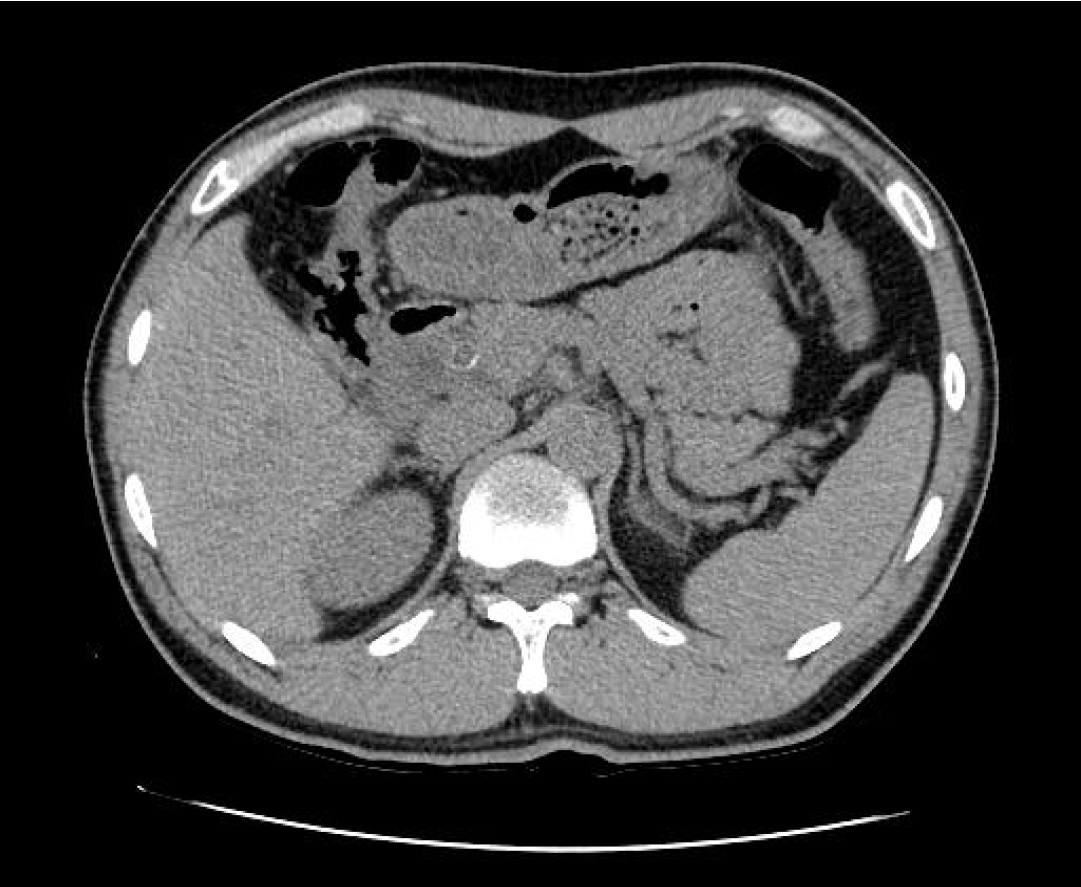
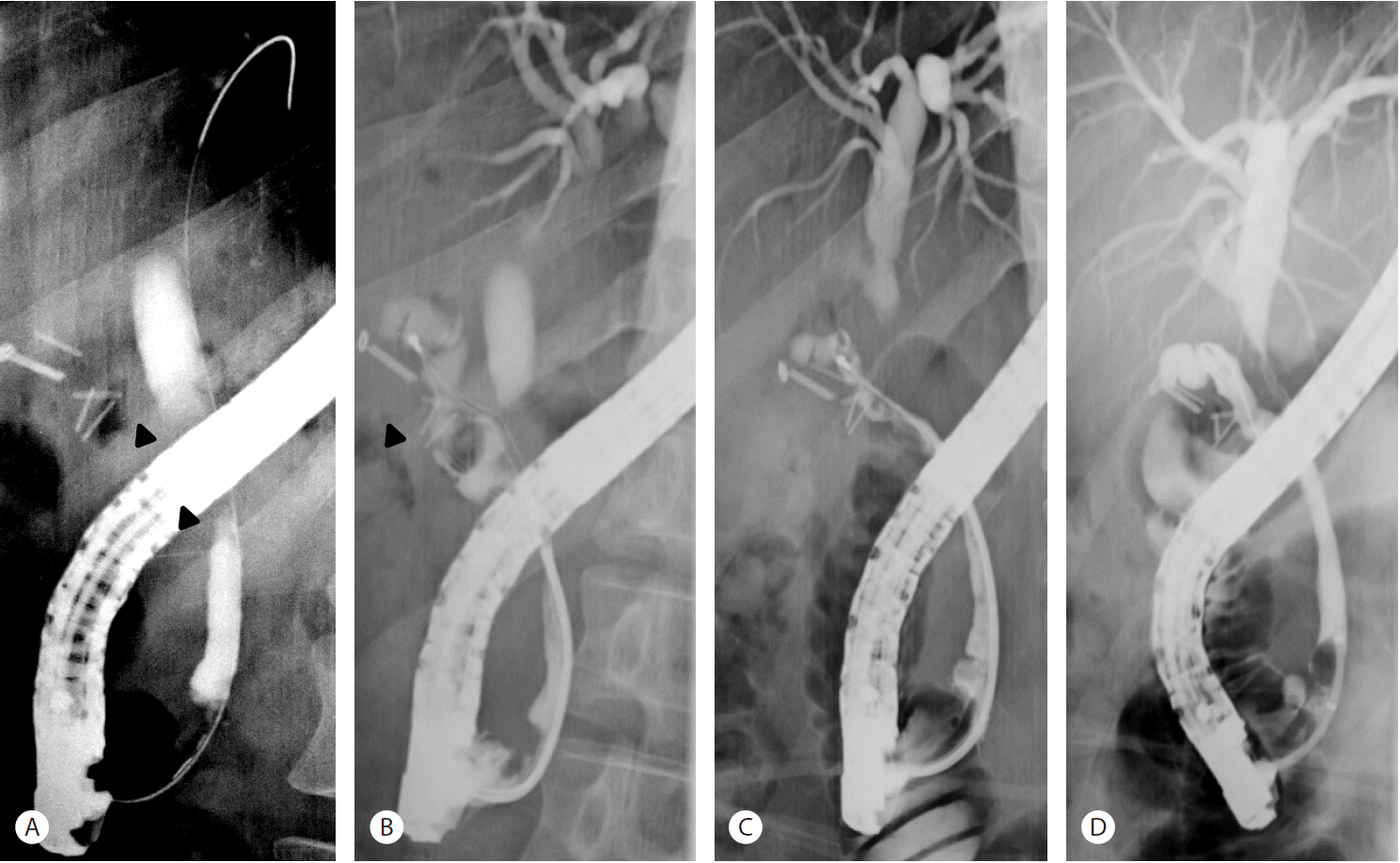
Due to the elevated bilirubin levels and non-normal liver function tests, abdominal CT was performed. The scan depicted a remnant cystic duct stone (0.8 cm) and cystic duct and extra- and intra-hepatic duct dilations (Fig. 1). Endoscopic retrograde cholangiopancreatography (ERCP) was performed, and a cholangiogram revealed a large impacted stone in a long and non-tortuous cystic duct stump with smooth luminal narrowing of the CHD and marked dilation of both intrahepatic ducts (Fig. 2A, 2B). A wire-guided retrieval basket (TrapezoidTMRX, Boston Scientific, Natick, Mass) was inserted inside the cystic duct, the stone was captured, and ML was performed (Fig. 2B). Stone fragments were removed using the basket.
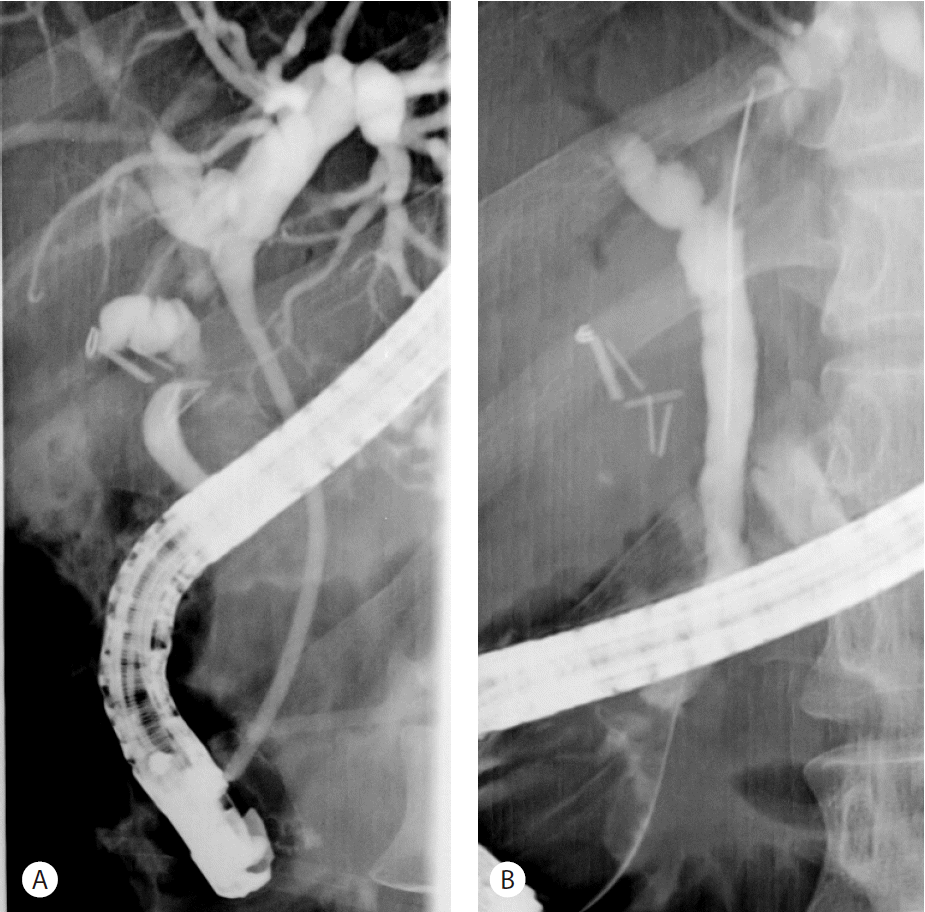
Two days later, follow-up cholangiography showed diminished dilatations of intrahepatic ducts, the CHD, and the cystic duct and small remnant filling defects corresponding to stone fragments in the cystic duct stump (Fig. 2C, 2D). These remnant fragments were completely removed using a basket and a retrieval balloon catheter, and a plastic stent was inserted to treat CHD stricture (Fig. 3A). Seven weeks later, the CHD narrowing had completely resolved and a balloon-occlusion cholangiogram showed no evidence of a retained bile duct stone (Fig. 3B).
DISCUSSION
MS is caused by an impacted stone in Hartmann’s pouch of the GB or cystic duct in close anatomic proximity to the common hepatic duct [1], and was first described by Mirizzi in 1948 [4]. According to the Csendes classification, MS can be categorized into four types based on the presence and extent of cholecystobiliary fistula. Type 1 involves simple external compression of the common hepatic duct by an impacted cystic duct stone. In type 2, a fistula involves under one third of the bile duct diameter. In types 3 and 4 a fistula involves from one to two thirds of the bile duct or more than two thirds or complete destruction of the wall of the bile duct, respectively [5,6].
Surgery is considered the treatment of choice for MS, and surgical strategies include open or laparoscopic cholecystectomy with T-tube placement and choledocholithotomy. The treatment of MS depends on the existence of a fistula. For type 1 MS a relatively straightforward operation is required, but for types 2, 3 and 4 MS interventions are more complex [1].
Improvements in endoscopic accessories and techniques have resulted in the developments of various endoscopic treatments for MS. England et al. in a retrospective study of 25 MS patients treated between March 1989 and June 1995 found that 13 patients were cured by endoscopic treatment with ML or extracorporeal shock wave lithotripsy [7].
A small number of reports have been issued on MS cases treated endoscopically in Korea. In 2007, it two cases of type 1 MS were treated endoscopically. The authors of this report advocated endoscopic intervention be considered prior to surgery in patients that refuse surgical treatment or present a high surgical complication risk [8].
When a patient who had received laparoscopic cholecystectomy presents recurrent right upper quadrant abdominal pain and laboratory studies shows obstructive jaundice, post-cholecystectomy MS should be considered, even after months or years after the operation [9]. Post-cholecystectomy MS caused by common bile duct obstruction by remnant cystic duct calculus after cholecystectomy is rare and considered a surgical indication. In a previous report, a patient with post-cholecystectomy MS initially underwent ERCP, but retrieval of the stone impacted in the cystic duct stump failed, and subsequently, he was treated successfully by laparoscopy [10]. In this previous case, the stone could not be removed by ERCP because of a narrow, tortuous cystic duct stump. On the other hand, Kodali et al. reported two cases of Post-choleccystectomy MS treated endoscopically by using ML and extraction basket after biliary decompression [9].
In our case, ERCP was possible because the cystic duct stump was wide and non-tortuous, and a remnant cystic duct stone was removed by ML during ERCP. In cases of post-cholecystectomy MS, repeat surgery probably increases risk of morbidity caused by post-operative scarring. In addition, extracorporeal shock wave lithotripsy combined with endoscopic management of impacted cystic duct stones in patients with high surgical risk has been reported [11]. Therefore, if possible, the endoscopic approach should be preferred.
Laser lithotripsy (LL) under peroral cholangioscopy (POC) such as Mother-baby scope, ultraslim endoscope or SpyGlass has also been used for the endoscopic treatment of post-cholecystectomy MS. Issa et al. reported two cases of endoscopic stone removal by SpyGlass guided laser lithotripsy [12]. In Korea, Laser lithotripsy via ultraslim endoscope has been published [13]. LL was chosen in these cases because endoscopic ML was not possible. However because of the high cost and rarity of such instruments, ML should be considered preferentially for patients with post-cholecystectomy MS.
When cystic duct stump diameter is large and non-tortuous, basket insertion into the cyst duct enables ML of even large stones in the cystic duct stump. In our case, we were able to remove the remnant cystic duct stone endoscopically without complication, and thus, we recommend ERCP with ML be considered in selected patients that develop type I MS after cholecystectomy.